Benzodiazepine Withdrawal: What You Need to Know
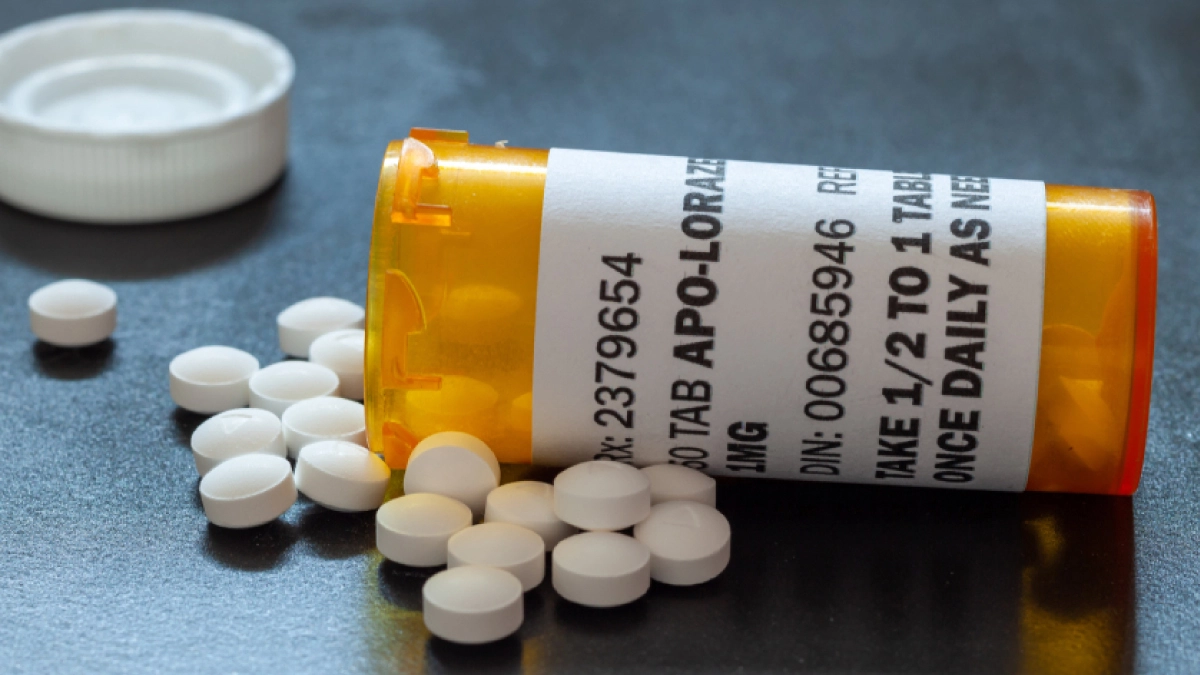
Benzodiazepine withdrawal happens when someone stops taking medicines like Xanax or Valium, often prescribed for anxiety or sleep problems. Suddenly quitting can lead to uncomfortable symptoms like body aches, insomnia, and even seizures.
It’s important to taper off these medications under a doctor’s guidance during the detox process to reduce withdrawal effects. If you or someone you know is facing benzodiazepine withdrawal, seek professional help for a safe and supportive approach. Remember, withdrawal is temporary, and with proper care, people can successfully transition to a benzodiazepine-free life.

Key Takeaways
Benzodiazepine withdrawal is tough; taper off with a doctor’s guidance to minimize discomfort. Here’s what you need to know:
- Benzodiazepine overdose incidents surged by 23.7 percent from 2019 to 2020.
- The benzodiazepine withdrawal timeline spans weeks to months, with medical care crucial for severe cases.
- Manage benzodiazepine withdrawal with gradual tapering, healthy choices, and emotional support.
For a secure withdrawal, consider The Haven Detox-Little Rock, prioritizing your safety and recovery. Call us today at (501) 271-3342.
Benzodiazepine Statistics Report
The surge in benzodiazepine-related overdose incidents, as reported by the Centers for Disease Control and Prevention (CDC), between 2019 and 2020 highlights the significant risks associated with benzodiazepine utilization in the United States.
The data reveals a sharp increase of 23.7 percent in benzodiazepine-related overdose incidents per 100,000 emergency department visits during this period. Furthermore, the number of benzodiazepine-related overdose cases rose significantly, going up by 21.0 percent.
These statistics underscore the urgency of addressing the complex interplay between benzodiazepines and other substances, especially opioids, and the need for comprehensive strategies to mitigate the associated risks.
Overdose Death Rate in The United States
It’s crucial to note that the statistics emphasize the severity of the benzodiazepine issue, stressing the importance of understanding the associated risks. High doses, especially of longer-acting benzodiazepines like Diazepam, heighten the potential for substance abuse and life-threatening outcomes.
Over a comparable period from April to June 2019 to the same months in 2020, overdose deaths linked to prescription benzodiazepines rose by 21.8 percent, while illicit benzodiazepine-related deaths skyrocketed by an alarming 519.6 percent.
Understanding the Addiction Cycle
Benzodiazepine addiction involves the intricate science of how these drugs impact our brains. When someone uses benzodiazepines, they affect a neurotransmitter called gamma-aminobutyric acid (GABA), which helps calm the brain. The problem lies in the short half-lives of certain benzodiazepines, leading to more frequent use for sustained relief.
People often get these drugs through prescriptions, especially for conditions like anxiety disorder. However, using them for extended periods, even as prescribed, can contribute to addiction.
Moreover, concurrent use of benzos and alcohol to intensify the euphoric effects can lead to dependence. That highlights the importance of cautious and informed prescription practices to mitigate potential substance abuse issues.
Factors Influencing the Benzodiazepine Addiction
Various factors, such as peer pressure and societal norms, can lead to the use of short-acting drugs and the transition to illicit substances, which influence the addiction cycle. Prescription benzodiazepines, designed to alleviate anxiety, may contribute to the cycle when used beyond recommended durations.
Understanding the interplay of these factors is crucial in addressing symptoms of the condition and developing interventions that break the cycle, promoting better mental health outcomes.
Symptoms of Benzodiazepine Withdrawal
Benzodiazepine withdrawal can bring about various symptoms, both short-term and long-term. Understanding these manifestations is crucial, especially considering the potential severity of withdrawal symptoms.
Short-Term Symptoms
In the short term, when someone stops taking benzodiazepines, they might experience intense withdrawal symptoms. These can include panic attacks, insomnia, physical discomfort, and the worsening of symptoms of anxiety.
Short-acting Benzos can lead to a more abrupt onset of withdrawal. The most common symptoms during this phase involve heightened stress levels, reflecting the body’s adjustment to the absence of benzodiazepine drugs. It’s essential for individuals undergoing withdrawal to be under medical supervision, as severe cases may require attention from medical professionals.
Long-Term Symptoms
Over the long term, withdrawal symptoms may persist, especially for those who have used benzodiazepines for a long time. Individuals withdrawing from long-acting benzodiazepines may face a prolonged period of acute withdrawal.
Mental health concerns, like intense anxiety attacks, depression, and cognitive impairments. In severe cases, individuals might experience severe symptoms such as intense cravings and suicidal thoughts, emphasizing the importance of recognizing signs of benzo withdrawal and seeking appropriate medical attention.
Benzodiazepine Withdrawal Timeline
Understanding the timeline of benzodiazepine withdrawal is like having a roadmap for the journey to feeling better. Let’s take a closer look at each phase:
Days 1-4
The first few days can be tough, with anxiety and sleep troubles taking the stage. During this stage, the body is adjusting to the absence of benzodiazepines.
Week 1
As we move into the first week, symptoms peak. During this phase, a person experiences intense anxiety, restlessness, and panic attacks. That is often the most challenging part and may require medical assistance.
Weeks 2-4
As we enter weeks 2-4, things start looking up. The intensity of symptoms reduces, and acute symptoms gradually improve. Yet, some discomfort and mood swings might linger.
Month 1-2
During the first and second months, emotional and physical symptoms ease. However, sleep disturbances and stress might still be around.
Months 3-6
From months 3 to 6, things keep getting better. Most people experience continued improvement, although occasional symptoms may appear.
Beyond Six Months
After six months, if there are any long-term symptoms like intense cravings for drugs, they might need ongoing support and monitoring.
Medical Assistance for Benzos Withdrawal Management
Stopping benzodiazepines can be tricky, and that’s why it’s crucial to get help from professionals for a safe and successful recovery.
Medical Detox
Drug and alcohol detox is the first step for addiction recovery. This essential process ensures that individuals navigate withdrawal under the careful observation of healthcare professionals.
This approach is particularly crucial for managing severe benzodiazepine withdrawal symptoms, as immediate medical attention is readily available if necessary. The focused care during medical detox includes prescription drugs and counseling to help ease the challenges associated with withdrawal.
Benzodiazepine Tapering
Benzodiazepine tapering is a gradual reduction strategy employed to minimize withdrawal symptoms and promote a safer transition toward independence from these medications. This structured process, conducted under medical supervision, systematically lowers the dosage over time.
Benzodiazepine tapering aims to mitigate the risk of severe withdrawal reactions and increase the likelihood of a successful and more comfortable recovery. The process is personalized to each individual, considering the specific benzodiazepine used, the duration of use, and the person’s overall health. Understanding the nuances of benzodiazepine tapering is crucial for fostering a supportive and effective withdrawal journey.
Role of Therapies and Support Groups During Recovery
Therapies and support groups play a pivotal role in addressing the mental and emotional dimensions of withdrawal, providing individuals with essential tools and a sense of community.
Therapy Programs
Therapeutic interventions, including cognitive-behavioral therapy (CBT), hold a pivotal position in addressing the mental health aspects of benzodiazepine withdrawal. Talking to mental health professionals is vital for those going through benzodiazepine withdrawal.
These professionals are like helpful friends who not only listen but also give practical advice on handling the emotional causes related to using benzodiazepines. They are there to support and guide you through this tough time, helping you understand your feelings better.
Support Groups
Being part of a support group is surrounded by people who understand what you’re going through. These groups create a feeling of togetherness, where people can discuss their challenges and successes. It’s like being in a caring community, allowing patients to share their experiences.
These group sessions help participants to share their challenges during or after recovery. When considering a support group, find one that aligns with your specific needs and circumstances.
Tips to Manage Withdrawal Symptoms
Withdrawal from substances like benzodiazepines can be challenging, but there are strategies to help manage symptoms and make the process more bearable.
Educate Yourself
Learn about the withdrawal process and potential symptoms. Knowledge empowers you to navigate challenges more effectively and understand what to expect.
Establish a Routine
Create a daily routine to provide structure and stability. Having a predictable schedule can help manage anxiety and create a sense of control during the withdrawal period.
Healthy Lifestyle Choices
Focus on maintaining a healthy lifestyle. That includes regular exercise, a balanced diet, and sufficient sleep, which can positively impact physical and mental well-being during withdrawal.
Emotional Support
Reach out to friends, family, or support groups. Having a strong support system is vital for emotional well-being. Sharing your feelings and experiences can provide comfort and encouragement.
Distraction Techniques
Engage in activities that distract from withdrawal symptoms. Hobbies, reading, or watching movies can redirect focus and ease discomfort.
Mindfulness and Relaxation
Practice mindfulness and relaxation techniques, such as deep breathing or meditation. These habits can help manage mental health and promote a sense of calm.
Frequently Asked Questions (FAQ)
What is benzodiazepine withdrawal syndrome?
Benzodiazepine withdrawal syndrome is when someone lowers or quits using drugs like Xanax or Valium. It brings symptoms like more worry, trouble sleeping, mood changes, and, in serious situations, even seizures.
This happens because the body is getting used to not having the benzodiazepine drugs it got used to before. If you or someone you know has these symptoms, get help from a doctor or healthcare professional.
How long does it take to detox from benzodiazepines?
The duration of benzodiazepine detox varies from person to person. Typically, the acute withdrawal phase lasts several weeks, with symptoms peaking around the first week. However, the overall detox process can extend for months, and some individuals may continue to experience occasional challenges even beyond six months.
Are there any home remedies to help cope with benzodiazepine withdrawal?
While medical supervision is crucial for benzodiazepine withdrawal, some home remedies may offer support. Engaging in relaxation techniques, maintaining a healthy lifestyle with exercise and a balanced diet, and staying connected with a support system can aid in managing symptoms. However, consulting with healthcare professionals is essential to ensure a safe and effective withdrawal process.
Take a Step Towards Recovery at The Haven Detox-Little Rock
Withdrawal can be challenging, and attempting it at home can be complicated and risky. That’s why The Haven Detox-Little Rock is here to provide a secure solution to you.
Our dedicated detox program ensures a safe and supportive environment, guiding you through the initial stages of recovery. Enhance your journey with our residential rehab services, offering a structured and caring environment. Our IV therapy delivers personalized treatments for a more comfortable detox process.
We are committed to supporting you every step of the way, promoting lasting recovery and wellness. Don’t hesitate to give us a call at (501) 271-3342 today.